
Chronic Pelvic Pain in Women
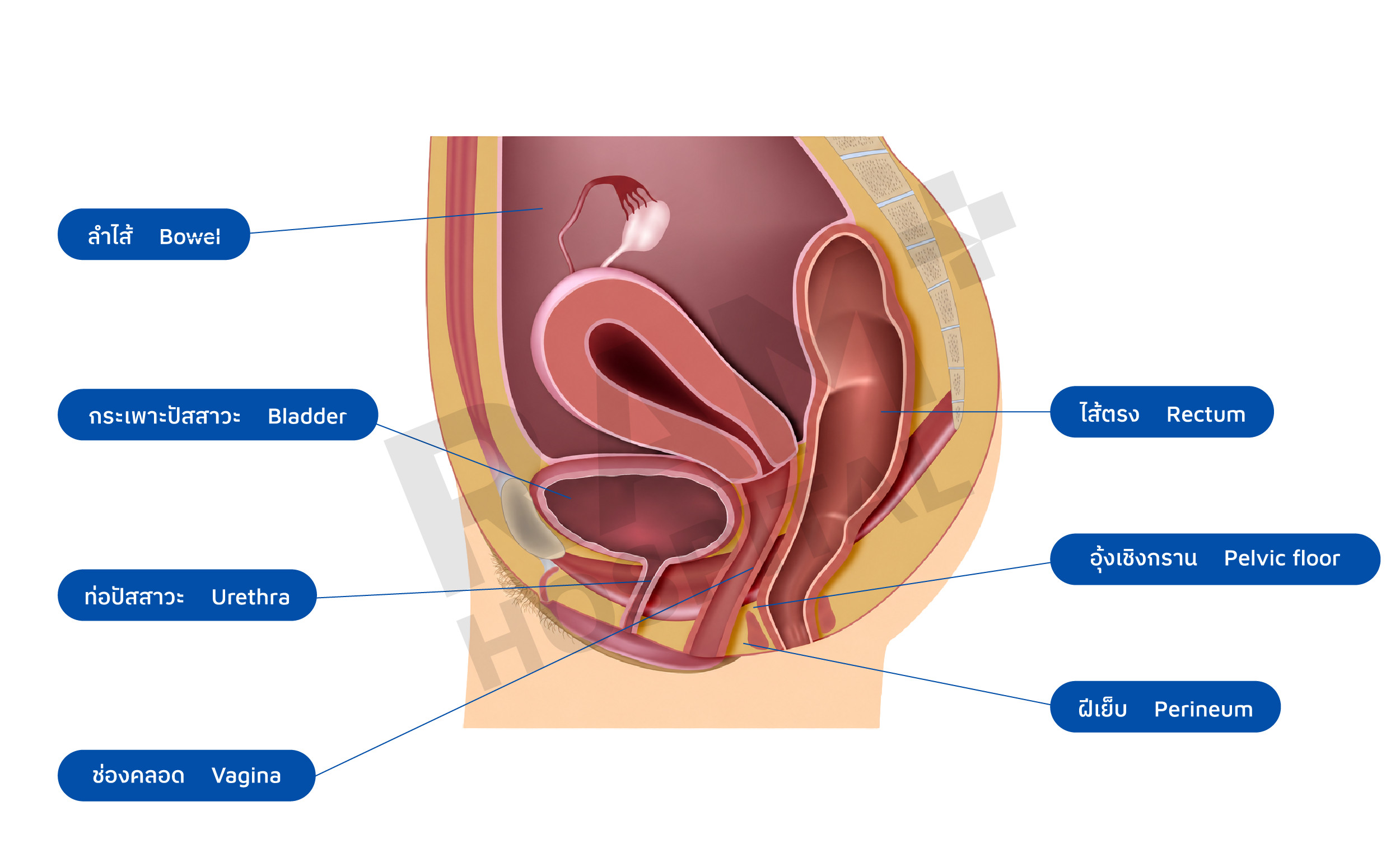
Chronic pelvic pain in women is defined as pain in the pelvic area caused by pelvic organs that lasts longer than 6 months1 (pelvic organs include the vagina, cervix, uterus, bladder, urethra, rectum, and muscles). The pain may be continuous, intermittent, or recurring. Sometimes it may be related to menstrual cycles, meals, urination, or sexual intercourse.
In the long term, this condition can lead to anxiety, fear, and stress, affecting work, education, family, and daily life. Therefore, it is crucial to receive an accurate diagnosis and proper care from a multidisciplinary team.
Causes of Chronic Pelvic Pain in Women?
1. Internal Organs (Visceral etiology)
- Gynecological Diseases: Such as Endometriosis, adnexal masses, pelvic inflammatory disease (PID), uterine fibroids, pelvic adhesions, etc.
- Gastrointestinal Diseases: Such as Irritable Bowel Syndrome (IBS), inflammatory bowel disease, colon cancer, diverticulitis, etc.
- Urinary System Diseases: Such as bladder cancer, urinary tract inflammation or complications, and Bladder Pain Syndrome (BPS).
2. Neuromusculoskeletal System (Neuromusculoskeletal)
Fibromyalgia, chronic muscle pain, postural syndrome, and abdominal wall syndrome.
3. Psychosocial Factors
- Physical, emotional, or sexual abuse; depression; anxiety; somatic symptom disorder; and substance use disorders.
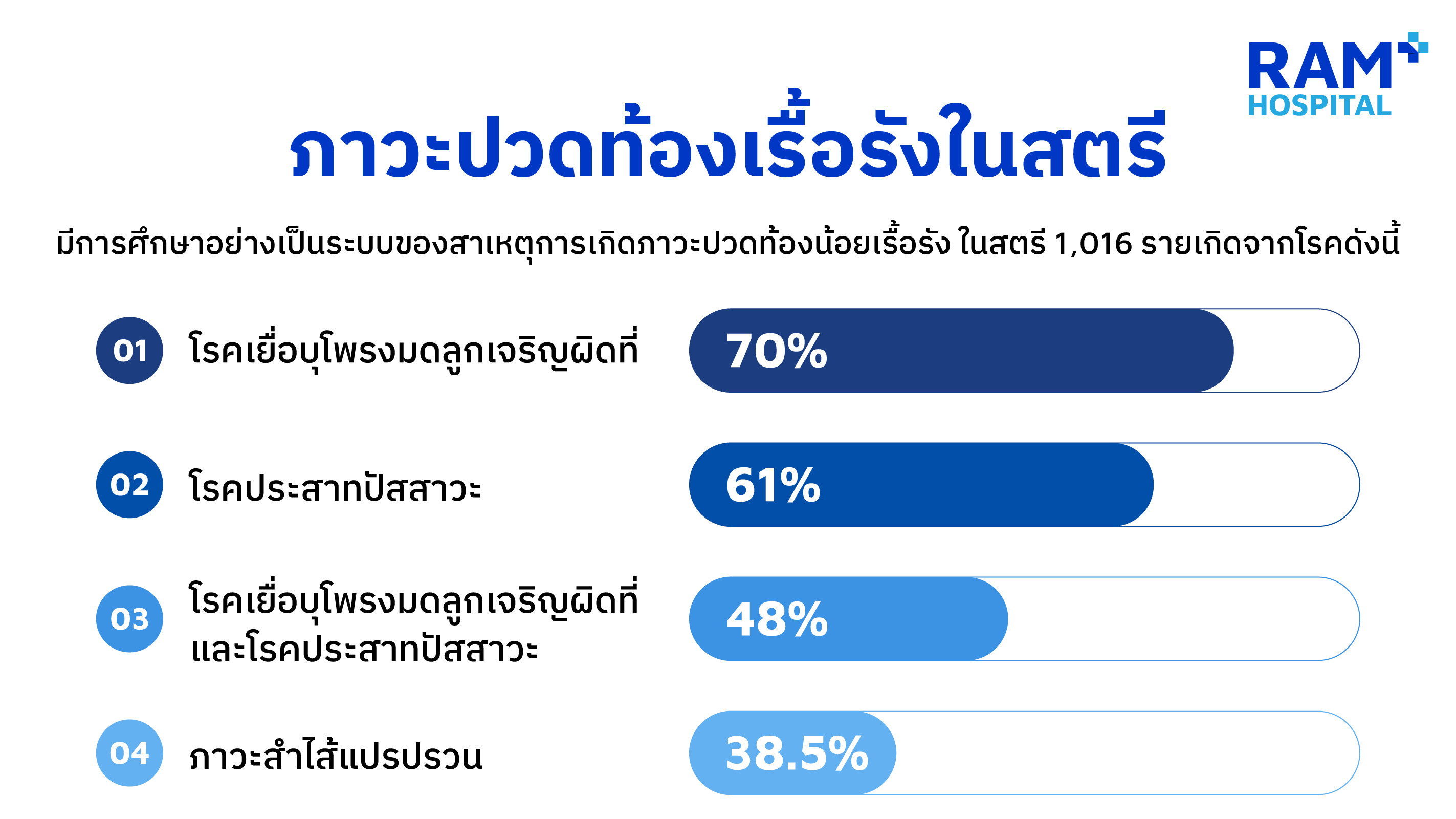
The prevalence of chronic pelvic pain in women is approximately 20%-60%.4-7 A systematic review of 1,016 women found that causes included endometriosis (70%), bladder pain syndrome (61%), and 48% had both conditions simultaneously.8 Some reports also found Irritable Bowel Syndrome in 38.5% of cases.9
Diagnosis of Chronic Pelvic Pain in Women
Since this condition often involves multiple co-occurring causes, diagnosis during the initial visit can be challenging. Patients should follow up regularly. Thus, taking a detailed history, physical examination, and diagnostic tests are essential, along with treatment by a multidisciplinary team.
Important Records for Patients to Bring
- Location of pain and onset duration.
- Pain triggers and relieving factors.
- Pain radiating to other areas or correlation with the menstrual cycle.
- Pain related to sexual intercourse.
- Correlation with meals or bowel movements.
- Urinary system symptoms.
- Physical exertion or posture, such as lifting heavy objects, exercising, or work habits.
Warning Signs to See a Doctor Immediately
- Post-coital bleeding (bleeding after sex).
- Abnormal bleeding in women over 40 years old.
- Bleeding or onset of pain after menopause.
- Unexplained weight loss.
- Palpable masses in the pelvis or abdomen.
- Rectal bleeding or blood in the urine.
Examinations and Considerations by the Doctor
Pelvic examination and initial laboratory tests include:
- Urine analysis.
- Testing for Sexually Transmitted Infections (STIs).
- Biopsy (tissue sample collection).
- Ultrasound or X-ray of the lower abdomen.
- Computerized Tomography (CT scan).
- Colonoscopy.
- Cystoscopy.
- Diagnostic Laparoscopy.

Treatment for Chronic Pelvic Pain in Women
The goal of treatment is to relieve pain and improve the patient's quality of life. Since chronic pelvic pain can arise from many factors, treatment options are diverse.
- Pain medication management.
- Physical therapy.
- Surgical intervention (Laparoscopic adhesiolysis).
- Cognitive Behavioral Therapy (CBT).
- Sex therapy.
 If you experience severe pain for an extended period, do not ignore it or assume it is normal for women. We recommend consulting a doctor for treatment based on professional diagnosis.
If you experience severe pain for an extended period, do not ignore it or assume it is normal for women. We recommend consulting a doctor for treatment based on professional diagnosis.
References
- Chronic Pelvic Pain: ACOG Practice Bulletin, Number 218. Obstet Gynecol. 2020. Mar;135(3):e98-e109
- Engeler DS, Baranowski AP, Dinis-Oliveira P, Elneil S, Hughes J, Messelink EJ, van Ophoven A, Williams AC., European Association of Urology. The 2013 EAU guidelines on chronic pelvic pain: is management of chronic pelvic pain a habit, a philosophy, or a science? 10 years of development. Eur Urol. 2013 Sep;64(3):431-9. [PubMed]
- Potts JM, Payne CK. Urologic chronic pelvic pain. Pain. 2012 Apr;153(4):755- 758. [PubMed]
- Learman LA, Gregorich SE, Schembri M, Jacoby A, Jackson RA, Kuppermann M. Symptom resolution after hysterectomy and alternative treatments for chronic pelvic pain: does depression make a difference? Am J Obstet Gynecol 2011;204:269.e1–9. (Level II-2)
- Williams RE, Hartmann KE, Sandler RS, Miller WC, Savitz LA, Steege JF. Recognition and treatment of irritable bowel syndrome among women with chronic pelvic pain. Am J Obstet Gynecol. 2005;192:761–7. (Level II-3)
- Cheng C, Rosamilia A, Healey M. Diagnosis of interstitial cystitis/bladder pain syndrome in women with chronic pelvic pain: a prospective observational study. Int Urogynecol J 2012;23:1361–6. (LevelII-3)
- Montenegro ML, Mateus-Vasconcelos EC, Rosa e Silva JC, Nogueira AA, Dos Reis FJ, Poli Neto OB. Importance of pelvic muscle tenderness evaluation in women with chronic pelvic pain. Pain Med 2010;11:224–8. (Level II-3)
- Tirlapur SA, Kuhrt K, Chaliha C, Ball E, Meads C, Khan KS. The ’evil twin syndrome’ in chronic pelvic pain: a systematic review of prevalence studies of bladder pain syndrome and endometriosis. Int J Surg 2013;11:233–7.
- Zondervan KT, Yudkin PL, Vessey MP, et al. Chronic pelvic pain in the community—symptoms, investigations, and diagnoses. Am J Obstet Gynecol. 2001;184(6):1149-1155.doi:10.1067/mob.2001.112904





If you experience severe pain for an extended period, do not ignore it or assume it is normal for women. We recommend consulting a doctor for treatment based on professional diagnosis.